We define a first ray amputation as an amputation of the phalanxes and of at least part of the metatarsus; therefore, we excluded patients who solely underwent. Boarder ray amputations do not significantly interfere with ambulation. In fact, amputation of the lateral two or even three rays often provides a functional weight-bearing foot. Amputation of the medial two and even three rays in special circumstances may provide a weight-bearing, sensitive, reasonably functional foot (See below).
Diabet Foot Ankle. 2012; 3: 10.3402/dfa.v3i0.12169.
Published online 2012 Jan 20. doi: 10.3402/dfa.v3i0.12169
PMID: 22396832
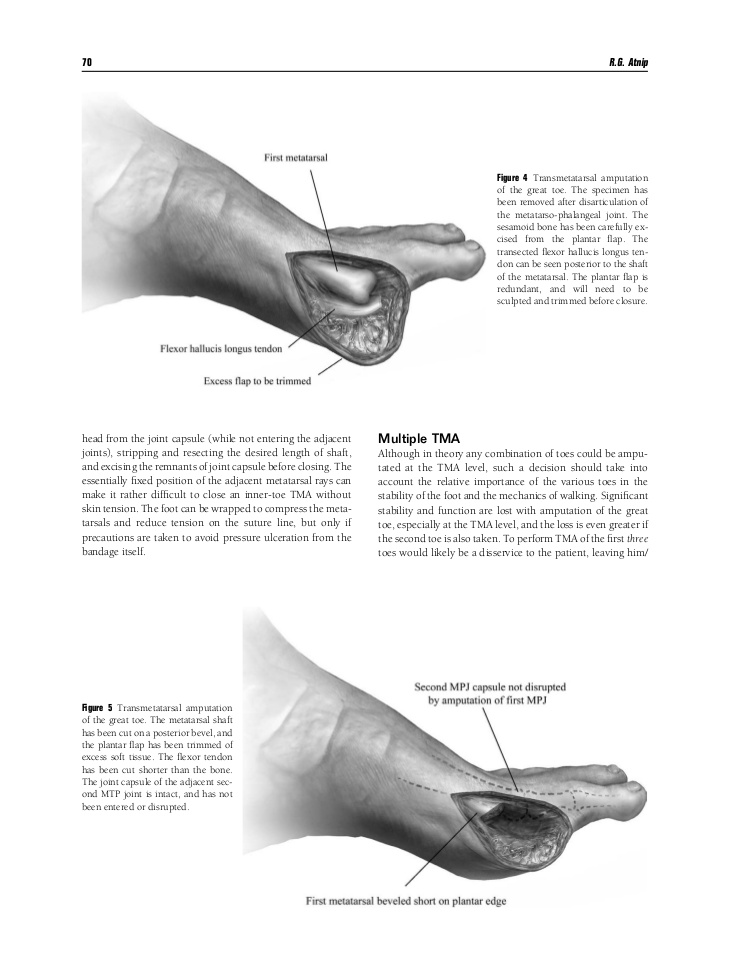
This article has been cited by other articles in PMC.
Abstract
Diabetes mellitus with peripheral sensory neuropathy frequently results in forefoot ulceration. Ulceration at the first ray level tends to be recalcitrant to local wound care modalities and off-loading techniques. If healing does occur, ulcer recurrence is common. When infection develops, partial first ray amputation in an effort to preserve maximum foot length is often performed. However, the survivorship of partial first ray amputations in this patient population and associated re-amputation rate remain unknown. Therefore, in an effort to determine the actual re-amputation rate following any form of partial first ray amputation in patients with diabetes mellitus and peripheral neuropathy, the authors conducted a systematic review. Only studies involving any form of partial first ray amputation associated with diabetes mellitus and peripheral sensory neuropathy but without critical limb ischemia were included. Our search yielded a total of 24 references with 5 (20.8%) meeting our inclusion criteria involving 435 partial first ray amputations. The weighted mean age of patients was 59 years and the weighted mean follow-up was 26 months. The initial amputation level included the proximal phalanx base 167 (38.4%) times; first metatarsal head resection 96 (22.1%) times; first metatarsal-phalangeal joint disarticulation 53 (12.2%) times; first metatarsal mid-shaft 39 (9%) times; hallux fillet flap 32 (7.4%) times; first metatarsal base 29 (6.7%) times; and partial hallux 19 (4.4%) times. The incidence of re-amputation was 19.8% (86/435). The end stage, most proximal level, following re-amputation was an additional digit 32 (37.2%) times; transmetatarsal 28 (32.6%) times; below-knee 25 (29.1%) times; and LisFranc 1 (1.2%) time. The results of our systematic review reveal that one out of every five patients undergoing any version of a partial first ray amputation will eventually require more proximal re-amputation. These results reveal that partial first ray amputation for patients with diabetes and peripheral sensory neuropathy may not represent a durable, functional, or predictable foot-sparing amputation and that a more proximal amputation, such as a balanced transmetatarsal amputation, as the index amputation may be more beneficial to the patient. However, this remains a matter for conjecture due to the limited data available and, therefore, additional prospective investigations are warranted.
Keywords: diabetic foot, hallux, ulceration, osteomyelitis, metatarsal, resection
Diabetes mellitus with peripheral sensory neuropathy is associated with a high risk for developing ulcerations to the distal aspect of the foot (–). Peak ambulatory forces are known to occur about the first ray, leaving this region prone to repetitive stresses and eventual breakdown (). Ulcerations at this level pose distinct barriers to conservative therapies due to the difficulty in properly offloading the wounds until healed nor keep them healed over time; inability to provide sufficient daily foot hygiene in debilitated patients; and compromised distal vascular inflow. Accordingly, many of these patients progress towards an amputation ().
The most appropriate index partial foot amputation level is difficult to accurately determine. However, in general, this involves complete resection of all necrotic, nonviable tissue while creating the most functional, durable, weight bearing residual foot that can be protected in a variety of shoe-gear types with or without bracing. Routinely, to preserve length and integrity to the remaining foot structures, for pathology about the hallux and first metatarsal, the most distal level of resection is usually chosen resulting in a partial first ray amputation. However, recent studies have questioned the reliability of this amputation level (–). In some circumstances, it has been shown that a more proximal index amputation level reduces the risk of re-ulceration and need for progressive levels of re-amputation (). To further investigate this topic, the authors undertook a systematic review of electronic databases to identify relevant material relating to the incidence of re-amputation following partial first ray amputation associated with diabetes mellitus and peripheral sensory neuropathy but without critical limb ischemia.
Methods
The authors performed a systematic review of electronic databases and relevant peer-reviewed sources including Infotrieve-Pubmed/MEDLINE (http://www4.infotrieve.com/newmedline/search.asp). The authors hand searched each identified manuscript for pertinent references. Only manuscripts that involved any form of partial first ray amputation associated with diabetes mellitus and peripheral neuropathy were included.
The authors performed the above systematic review with no restriction on date or language, using an inclusive text word query ‘First ray’ OR ‘Hallux’ AND ‘Amputation’ OR ‘Resection’ AND ‘Diabetes’ AND ‘Neuropathy’ where the all upper-case words represent the Boolean operators employed. Every manuscript was reviewed in their entirety and consensus was met for final inclusion with the lead author being the moderator.
Results
The search for potentially eligible information for inclusion in the systematic review yielded a total of 24 references. All references identified were obtained and reviewed by the authors in September 2010 with additional papers being identified and obtained in May 2011. After considering all of the potentially eligible references, five (20.8%) met our inclusion criteria and were included in this study. Specifically, one evidence-based medicine level I study () and four level IV studies met our inclusion criteria (, , , ) (Table 1). The methodological quality of the included studies was generally fair, although one study was designed to be prospective with randomization of patients.
Table 1
| Author (Year) | Patients (Number) | Age (Range) | Sex | Original amputation level | More proximal amputations (%) | End stage amputation level (Number; %) | Follow-up (Months) [Range] |
|---|---|---|---|---|---|---|---|
| Sizer (3) (1972) | 206 | 56.8 | N/A | Proximal Phalanx Base (166) | 8 (3.9%) | Transmetatarsal | N/A |
| 1st Metatarsal Head (40) | 7 (3.4%) | (15; 7.3%) | |||||
| Total: 15 (7.3%) | |||||||
| Johnson (4) (1987) | 1 | 29 | 1M | Proximal Phalanx Base | 0 | N/A | 9 |
| Murdoch (5) (1997) | 90 | 56.2 (31–83) | 70M | Partial Hallux (19) | 14 (15.6%) | Digital (9; 10%) | 36 |
| Transmetatarsal (2; 2.22%) | |||||||
| Below Knee (3; 3.33%) | |||||||
| 58.7 (45–74) | 20F | 1st MPJ Disarticulation(36) | 24 (26.7%) | Digital (10; 11.11%) | |||
| Transmetatarsal (5/5.56%) | |||||||
| Below Knee (9; 10%) | |||||||
| 1st Metatarsal Head Resection (12) | 7 (7.8%) | Digital (5; 5.6%) | |||||
| Transmetatarsal (1; 1.1%) | |||||||
| Below Knee (1; 1.1%) | |||||||
| Midshaft (22) | 9 (10%) | Digital (2; 2.2%) | |||||
| Transmetatarsal (2; 2.2%) | |||||||
| Below Knee (5; 5.6%) | |||||||
| Metatarsal Base (1) | 0 | ||||||
| Total: 54 (60%) | |||||||
| Dalla-Paola (6) (2003) | 89 | 66.3 | 63M | 1st Metatarsal Head (44) | 8 total (8.99%) | Digital (6; 6.7%) | 16.4 |
| 26F | Midshaft (17) | Transmetatarsal (1; 1.1%) | [7–28] | ||||
| Metatarsal Base (28) | LisFranc (1; 1.1%) | ||||||
| Ahmed (7) (2010) | 49/49 | 58 | 92M | Fillet Flap Hallux (32) | 0 | Transmetatarsal (2; 4.1%) | N/A |
| 30F | 1st MPJ Disarticulation (17) | 9 (18.4%) | Below Knee (7; 14.3%) | ||||
| Total: 9 (18.4%) |
F, female; M, male; MPJ, metatarsal-phalangeal joint; N/A, not applicable.
A total of 435 patients with a weighted mean age of 59 years and a weighted mean follow-up of 26 months, were included. The index amputation level included the proximal phalanx base 167 (38.4%) times; first metatarsal head resection 96 (22.1%) times; first metatarsal-phalangeal joint disarticulation 53 (12.2%) times; first metatarsal mid-shaft 39 (9%) times; hallux fillet flap 32 (7.4%) times; first metatarsal base 29 (6.7%) times; and partial hallux 19 (4.4%) times. The incidence of re-amputation was 19.8% (86/435). The end stage, most proximal level, following re-amputation was an additional digit 32 (37.2%) times; transmetatarsal 28 (32.6%) times; below-knee 25 (29.1%) times; and LisFranc 1 (1.2%) time.
Discussion
The purpose of this systematic review was to evaluate the incidence of re-amputation following partial first ray amputation associated with diabetes mellitus and peripheral neuropathy. The goal of any amputation is complete eradication of nonviable tissue optimizing the host's healing potential while reducing the risk for further breakdown and the need for repeated surgical intervention. To obtain this goal, the level of amputation at initial intervention needs to be chosen with due diligence (–, ). As shown in this study, at a mean follow-up of only 26 months, one out of every five patients who undergo a partial first ray amputation will require a more proximal level re-amputation due to the development of a neuropathic ulceration. Interestingly, the additional level of resection did not occur more proximally along the first ray itself but rather involved a separate digit 32 (37.2%) times, transmetatarsal level 28 (32.6%) times, below-knee level 25 (29.1%) and LisFranc level 1 (1.2%) time.
Weaknesses of this study include the fact that the search for manuscripts that met the inclusion criteria was performed through electronic databases. It is possible that pertinent references may have been inadvertently overlooked or excluded. Moreover, the search did not include a number of potential electronic databases. A more expansive search may have yielded supplementary references for inclusion. Furthermore, the data included in this systematic review spanned nearly 30 years during which the approaches available to treat diabetic neuropathic foot ulceration as well as forefoot amputations has undergone significant change.
However, review of the incidence of amputation is not appreciably different between the earliest and most recent manuscript included in our systematic review. In addition, the inclusion criteria were quite narrow. This produced a small number of manuscripts for evaluation. Many studies included partial first ray amputations along with an additional digit or other surgical intervention. Also, contralateral limb surgery was also performed along with the initial amputation in many studies. Finally, it is possible that some amputations were the result of critical limb ischemia and not solely peripheral sensory neuropathy. This would obviously affect both index amputation healing as well as level of subsequent amputation. With such variety in the description of the procedure, the authors believed it was necessary to define narrow inclusion criteria to assure that one procedure was critically analyzed. This did, however, result in a smaller number of manuscripts to be included in the review.
After a systematic review of peer-reviewed literature, the incidence of re-amputation following partial first ray amputation associated with diabetes mellitus and peripheral neuropathy was determined to be 19.8%. This reveals a relatively high rate of re-amputation in a high-risk subset of patients and additional reviews should be undertaken to further evaluate the continued utility of the partial first ray amputation associated with diabetes mellitus with peripheral neuropathy. Furthermore, reviews evaluating the utility and durability of the more proximal level amputations, such as a well-balanced transmetatarsal amputation (–), need to be initiated. Only then can a critical comparison, preferably prospective and through appropriately weighted design, be undertaken to define which level of amputation in the distal foot results in the lowest incidence of ulceration and/or re-amputation while maintaining the highest level of function.
Conclusion
A systematic review of electronic databases to determine the incidence of re-amputation following first ray amputation associated with diabetes mellitus and peripheral sensory neuropathy was undertaken. Based on the inclusion criteria, a total of five studies (20.8%) were included in the analysis. All of the studies had been published in peer-reviewed journals, although they were of methodologically fair design. The results of these studies reveal a high incidence of re-amputation of 19.8%. Therefore, given the available data, additional prospective investigations are warranted, especially in evaluation and comparison of various levels of partial foot amputation.
Conflict of interest and funding
The authors have received no funding or benefits from industry or elsewhere to conduct this literature review.
References
1. Lavery LA, Lavery DC, Quebedeax-Farnham TL. Increased foot pressures after great toe amputation in diabetes. Diabetes Care. 1995;18:1460–2. [PubMed] [Google Scholar]
2. Van Damme H, Rorive M, Martens De Noorthout B, Quaniers J, Scheen A, Limet R. Amputations in diabetes patients: a plea for footsparing surgery. Acta Chir Belg. 2001;101:123–9. [PubMed] [Google Scholar]
3. Sizer JS, Wheelock FC. Digital amputations in diabetic patients. Surgery. 1972;72:980–9. [PubMed] [Google Scholar]
4. Johnson MK, Rybczynski J, Kanat IO. Hallux amputation for diabetic osteomyelitis. J Foot Surg. 1987;26:141–8. [PubMed] [Google Scholar]
5. Murdoch DP, Armstrong DG, Dacus JB, Laughlin TJ, Morgan CB, Lavery LA. The natural history of great toe amputations. J Foot Ankle Surg. 1997;36:204–8. [PubMed] [Google Scholar]
6. Dalla Paola L, Faglia E, Caminiti M, Clerici G, Ninkovic S, Deanesi V. Ulcer recurrence following first ray amputation in diabetic patients: a cohort prospective study. Diabetes Care. 2003;26:1874–8. [PubMed] [Google Scholar]
7. Ahmed ME, Tamimi AO, Mahadi SI, Widatalla AH, Shawer MA. Hallux ulceration in diabetic patients. J Foot Ankle Surg. 2010;49:2–7. [PubMed] [Google Scholar]
8. Hodge MJ, Peters TG, Efird WG. Amputations of the distal portion of the foot. South Med J. 1989;82:1138–42. [PubMed] [Google Scholar]
9. Light JT, Jr, Rice JC, Kerstein MD. Sequelae of limited amputation. Surgery. 1988;103:294–9. [PubMed] [Google Scholar]
10. Quebedeaux TL, Lavery LA, Lavery DC. The development of foot deformities and ulcers after great toe amputation in diabetes. Diabetes Care. 1996;19:165–7. [PubMed] [Google Scholar]
11. Eneroth M, Apelqvist J, Stenström A. Clinical characteristics and outcome in 223 diabetic patients with deep foot infections. Foot Ankle Int. 1997;18:716–22. [PubMed] [Google Scholar]
12. Adler AI, Boyko EJ, Ahroni JH, Smith DG. Lower-extremity amputation in diabetes. The independent effects of peripheral vascular disease, sensory neuropathy, and foot ulcers. Diabetes Care. 1999;22:1029–35. [PubMed] [Google Scholar]
13. Rayman G, Krishnan ST, Baker NR, Wareham AM, Rayman A. Are we underestimating diabetes-related lower-extremity amputation rates? Results and benefits of the first prospective study. Diabetes Care. 2004;27:1892–6. [PubMed] [Google Scholar]
14. Armstrong DG, Lavery LA, Harkless LB, Van Houtum WH. Amputation and reamputation of the diabetic foot. J Am Podiatr Med Assoc. 1997;87:255–9. [PubMed] [Google Scholar]
15. Izumi Y, Satterfield K, Lee S, Harkless LB. Risk of reamputation in diabetic patients stratified by limb and level of amputation: a 10-year observation. Diabetes Care. 2006;29:566–70. [PubMed] [Google Scholar]
16. Kanade R, Van Deursen R, Burton J, Davies V, Harding K, Price P. Re-amputation occurrence in the diabetic population in South Wales, UK. Int Wound J. 2007;4:344–52. [PubMed] [Google Scholar]
17. Nehler MR, Whitehall TA, Bowers SP, Jones DN, Hiatt WR, Rutherford RB, et al. Intermediate-term outcome of primary digit amputations in patients with diabetes mellitus who have forefoot sepsis requiring hospitalization and presumed adequate circulatory status. J Vasc Surg. 1999;30:509–518. [PubMed] [Google Scholar]
18. Baddeley RM, Fulford JC. A trial of conservative amputations for lesions of the feet in diabetes mellitus. Brit J Surg. 1965;52:38–43. [PubMed] [Google Scholar]
19. Moss SE, Klein R, Klein BE. The 14-year incidence of lower-extremity amputation in a diabetic population. The Wisconsin epidemiologic study of diabetic retinopathy. Diabetes Care. 1999;22:951–9. [PubMed] [Google Scholar]
20. Van Houtum WH, Lavery LA. Outcomes associated with diabetes-related amputations in The Netherlands and in the state of California, USA. J Intern Med. 1996;240:227–31. [PubMed] [Google Scholar]
21. Siitonen OI, Niskanen LK, Laasko M, Siitonen JT, Pyöräiä K. Lower-extremity amputations in diabetic and nondiabetic patients. A population-based study in eastern Finland. Diabetes Care. 1993;16:16–20. [PubMed] [Google Scholar]
22. Ebskov B, Josephsen P. Incidence of reamputation and death after gangrene of the lower extremity. Prosthet Orthot Int. 1980;4:77–80. [PubMed] [Google Scholar]
23. Kahn O, Wagner W, Bessman AN. Mortality of diabetic patients treated surgically for lower limb infection and or gangrene. Diabetes. 1974;23:287–92. [PubMed] [Google Scholar]
24. Iannucci AJ, Channell RW, King PL, Farrell DJ. Spontaneous fractures of the lesser metatarsals secondary to an amputated hallux and peripheral neuropathy. J Foot Surg. 1987;26:66–71. [PubMed] [Google Scholar]
25. Roukis TS, Singh N, Andersen CA. Preserving functional capacity as opposed to tissue preservation in the diabetic patient: a single institution experience. Foot Ankle Spec. 2010;3:177–83. [PubMed] [Google Scholar]
26. Roukis TS. Flexor hallucis longus and extensor digitorum longus tendon transfers for balancing the foot following transmetatarsal amputation. J Foot Ankle Surg. 2009;48:398–401. [PubMed] [Google Scholar]
27. Schweinberger MH, Roukis TS. Intramedullary screw fixation for balancing of the dysvascular foot following transmetatarsal amputation. J Foot Ankle Surg. 2008;47:594–7. [PubMed] [Google Scholar]
28. Schweinberger MH, Roukis TS. Soft-tissue and osseous techniques to balance forefoot and midfoot amputations. Clin Podiatr Med Surg. 2008;25:623–39. [PubMed] [Google Scholar]
29. Schweinberger MH, Roukis TS. Surgical correction of soft-tissue ankle equinus contracture. Clin Podiatr Med Surg. 2008;25:571–85. [PubMed] [Google Scholar]
Articles from Diabetic Foot & Ankle are provided here courtesy of Taylor & Francis
Diabet Foot Ankle. 2013; 4: 10.3402/dfa.v4i0.21288.
Published online 2013 Jul 16. doi: 10.3402/dfa.v4i0.21288
PMID: 23869251
This article has been cited by other articles in PMC.
Abstract
Minor amputations in diabetic patients with foot complications have been well studied in the literature but controversy still remains as to what constitutes successful or non-successful limb salvage. In addition, there is a lack of consensus on the definition of a minor or distal amputation and a major or proximal amputation for the diabetic population. In this article, the authors review the existing literature to evaluate the efficacy of minor amputations in this selected group of patients in terms of diabetic limb salvage and also propose several definitions regarding diabetic foot amputations.
Keywords: diabetic foot infections, amputations, diabetic neuropathy
One of the most valuable strategies for managing the diabetic foot is to prevent the development of foot complications since neuropathic foot ulceration can often lead to loss of a limb due to a major amputation, i.e. below the knee amputation (BKA). For this to be achieved, patients diagnosed with diabetes mellitus must be subjected to early annual foot screening programs (). Once a diabetic foot complication has developed, the next best strategy is to treat this complication early in a hospital setting by a multidisciplinary diabetic foot team (, 3). The objective of early and efficacious treatment is to achieve limb salvage in order to avoid the loss of a limb from a major amputation.
However, controversy still remains in the existing literature as to what constitutes successful or non-successful diabetic limb salvage as well as a definition of a minor or distal amputation and a major or proximal amputation. Izumi et al. () referred to a Syme amputation as major amputation and in a study by Evans et al. (), no Syme amputation was included where the authors compared forefoot and midfoot amputations to BKA. Svensson et al. () compared a BKA group with an above-the-ankle amputation.
Based on the current literature, the authors propose the following definitions regarding the terms of distal or minor amputation versus a proximal or major amputation (Table 1). In addition, the terms successful versus non-successful amputations for diabetic limb salvage are still needed to be defined based on the amputation level, functionality, recurrence of ulceration and/or amputation and in larger cohort studies. The ASEAN Plus Expert Group Forum for the Management of Diabetic Foot Wounds that was held in Singapore on November 10, 2002, developed clinical practice guidelines for the management of diabetic foot wounds and has adopted these criteria. The senior author of this article is the chairman of this forum and the workgroup includes two experts each from Indonesia, Malaysia, Philippines, Singapore, Sri Lanka, and Thailand.
Table 1
Classification of various diabetic foot surgeries into major or minor amputations.
| Amputation level | Distal or minor amputation (tibial weight-bearing stump is preserved) | Proximal or major amputation (tibial weight-bearing stump cannot be preserved) |
|---|---|---|
| Forefoot | Toe disarticulation | |
| Ray (metatarsal and toe) | ||
| Transmetatarsal | ||
| Midfoot | Lisfranc | |
| Chopart | ||
| Hindfoot | Syme | |
| Boyd | ||
| Pirogoff | ||
| Modified Pirogoff | ||
| Trans-tibial | Below the knee | |
| Through the knee | Gritti stokes | |
| Trans-femoral | Above the knee | |
| Hip | Hip disarticulation |
The first amputation for patients with diabetic foot complications should preferably be a minor (distal) amputation. When a major (proximal) amputation, such as BKA is performed, the mortality rate is significantly higher than when a minor amputation (such as ray) is performed (, ). Izumi et al. () reported a significant difference in mortality with the hazard rate being 1.6 times in major amputees compared to ray amputees. Evans et al. () found that 80% of minor amputees were still alive after 2 years; 73% of minor amputees preserved their lower limb; and 64% were still fully ambulatory. In the BKA group, 52% died within 2 years and only 64% of patients ambulated with a prosthetic limb (). Svensson et al. (), in a study of 410 patients undergoing minor amputations, found that limb salvage could be achieved in almost two-thirds of patients.
Distal or minor amputations for the diabetic foot
Forefoot amputation
Toe disarticulations can be quite challenging for the surgeon when dealing with the remaining cartilage of the involved metatarsal head and possible complications of residual osteomyelitis. Atway et al. () reported a positive margin culture in three out of 13 patients (23.1%) who had a toe disarticulation.
Ray amputation, which involves the excision of the toe and part of the metatarsal, provides a more viable option of ensuring an adequate surgical debridement of the septic margins. Indications may include a wet or dry gangrene of a toe, osteomyelitis of the metatarsal head and/or proximal phalanx, septic arthritis of the metatarsophalangeal joint (MTPJ) and gross infection of the toe. Suggested inclusion criteria for this type of amputation may include one or two palpable pedal pulses, ankle brachial index (ABI) ≥ 0.8 and toe brachial index ≥ 0.7.
Borkosky et al. () reported a 19.8% incidence of re-amputation in patients with diabetes and peripheral sensory neuropathy undergoing partial first ray resection. Wong et al. (9) reported a 70% success rate of ray amputation in a cohort of 150 patients with diabetic foot problems. Absence of pulses, delayed capillary filling, high erythrocyte sedimentation rate, high creatinine and high neutrophil counts were found to be predictive factors for a poor clinical outcome (9).
Indications for transmetatarsal (TMA) amputation may include wet or dry gangrene involving only the forefoot and/or infection involving the forefoot while the inclusion criteria are the same as those mentioned above required for a ray amputation. Brown et al. () in a retrospective study of 21 patients reported a high functioning level and durability of the stump in patients undergoing TMA and concluded that it provides an ambulatory advantage. However, TMA has been reported to give significant complication and failure rates. Anthony et al. () reported 82% of patients requiring further surgery while Pollard et al. () reported a wound-healing rate of only 54%.
Amputation at the metatarsal level causes a muscular imbalance due to resultant equinovarus deformity from unopposed action of gastrocnemius, tibialis anterior, and tibialis posterior tendons, which is coupled with the deficiency of the muscular tension of the extensor tendons (). Adjunctive soft tissue procedures such as tendo-Achilles lengthening and split tibialis anterior tendon transfer for muscular imbalance are needed to correct for the equinovarus deformity. In addition, special footwear modifications are needed to reduce complication rates ().
Midfoot amputation
Lisfranc's disarticulation is a disarticulation through the tarsometatarsal joint, while Chopart's disarticulation is a disarticulation through the talonavicular and calcaneocuboid joints leaving only the hindfoot (talus and calcaneum) behind (Fig. 1). These amputations are rarely performed in diabetic foot infections due to high failure rate and the proximity of infected tissue to the heel pad. However, Brown et al. () reported high ambulatory levels for Chopart's disarticulation in his series of 10 patients. This suggests a favorable advantage for patients to ambulate if peri-operative and post-operative complications could be avoided.
Diagram demonstrating the Lisfranc's and Chopart's joints.
Elsharawy () studied the outcome of midfoot amputations in diabetic gangrene in his cohort study of 32 patients. There were wound-healing complications in eight patients (27%), which necessitated a BKA. Successful limb salvage, which was defined as a stump with functional ambulation, was seen in only 30 patients (67%) (). A systematic review of the existing literature was conducted by Schade et al. to identify any factors that may be associated with a successful Chopart amputation in diabetic foot problems (). The efficacy of tendinous and/or osseous balancing could not be assessed due to lack of comparable techniques, highlighting the paucity of literature in this field ().
Hindfoot amputation
This category included the amputations as shown in Table 1 and has the indications and inclusion criteria as mentioned in the forefoot amputation category. Syme's amputation has been advocated for trauma cases (); however, with strict selection criteria, Syme's amputation can give good results in patients with diabetic foot infections (). It is well known that Syme's amputation should be reserved for patients with at least a palpable posterior tibial pulse and an ankle-brachial index of more than 0.5 (–). There are several disadvantages to performing a Syme's amputation. This includes instability of the calcaneal flap due to poor adherence of the soft tissue of the calcaneal flap to the tibial surface. Also, the dissection of the calcaneum from the underlying flap in a Syme's amputation may lead to devascularization of the flap (). A third disadvantage is that the Syme's amputation with excision of the calcaneum leads to a shorter stump. This causes significant limb length discrepancy, which makes walking barefoot difficult ().
The Boyd and Pirogoff amputation is designed to give better results than the Syme's amputation (–). In the Boyd and Pirogoff amputation, the tibio-calcaneal bony fusion gives added stability to the flap. There is also reduced devascularization of the flap since the calcaneum is not dissected. Limb length discrepancy is also minimized. Along with a stable full weight-bearing stump due to the tibio-calcaneal fusion, the additional length makes it easier for the patient to walk without a prosthesis (). In addition, a part of the medial and lateral malleolus preserved in these amputations makes it easier for prosthesis to be fitted. The prosthesis can be worn with less friction and is more rotationally stable compared to a Syme's prosthesis.
Nather et al. (25) reported good outcomes in all six patients undergoing Pirogoff's amputation (Figs. 2 and and3)3) followed up over a minimum of 1 year. Strict selection criteria included a palpable posterior tibial pulse, ABI of more than 0.7, Hemoglobin level of more than 10 g/dL and serum albumin level of more than 30 g/L (25). The outcome of Pirogoff's amputation is still controversial. The cost of the prosthesis for Pirogoff's amputation is similar compared to that of a BKA. In terms of function, the Pirogoff's amputation is a weight-bearing stump. This has many advantages, including load sharing, which reduces the friction between the stump and the prosthesis and patients are able to ambulate short distances without wearing their prostheses. However, as the supramalleolar stump is bulbous in shape, it is difficult to fit a prosthesis for the Pirogoff's amputation.
Radiographic views of a modified Pirogoff's stump at 6-month follow-up.
Clinical picture of a well-healed stump at 6-month follow-up.
Discussion
Further sub-categorizing of operative methods is useful for being more accurate in the level of amputation for diabetic limb salvage surgery. Different levels of amputations provide unique problems in function and prostheses fitting due to the anatomical differences in each region. Problems in the midfoot will require muscle tendon transfers to ensure a well-functioning stump. Even though at times when a BKA stump is a better option for ambulation, patients may still choose a limb salvage operation in the attempt to preserve any remaining limb length.
Conclusion
Minor amputations in patients with diabetic foot problems have been shown to be effective in limb salvage and reducing morbidity and mortality in patients. The authors have proposed several definitions regarding diabetic foot amputations while further studies are needed for a consensus on the definition on a successful versus non-successful diabetic limb salvage surgery.
Conflict of interest and funding
The authors have received no funding or benefits from industry to conduct this study.
References
1. Nather A, Chionh SB, Tay PL, Aziz Z, Teng JW, Rajeswari K, et al. Foot screening for diabetics. Ann Acad Med Singapore. 2010;39:472–5. [PubMed] [Google Scholar]
2. Nather A, Siok Bee C, Keng Lin W, Xin-Bei Valerie C, Liang S, Tambyah PA, et al. Value of team approach combined with clinical pathway for diabetic foot problems: a clinical evaluation. Diabet Foot Ankle. 2010;1:5731.[PMC free article] [PubMed] [Google Scholar]
3. Nather A, editor. London: World Scientific Publishing; 2013. The diabetic foot; pp. 629–52. [Google Scholar]
4. Izumi Y, Satterfield K, Lee S, Harkless LB, Lavery LA. Mortality of first-time amputees in diabetics: a 10-year observation. Diabetes Res Clin Pract. 2009;83:126–31. [PubMed] [Google Scholar]
5. Evans KK, Attinger CE, Al-Attar A, Salgado C, Chu CK, Mardini S, et al. The importance of limb preservation in the diabetic population. J Diabetes Complications. 2011;25:227–31. [PubMed] [Google Scholar]
6. Svensson H, Apelqvist J, Larsson J, Lindholm E, Eneroth M. Minor amputation in patients with diabetes mellitus and severe foot ulcers achieves good outcomes. J Wound Care. 2011;20:261–2. 264, 266. [PubMed] [Google Scholar]
7. Atway S, Nerone VS, Springer KD, Woodruff DM. Rate of residual osteomyelitis after partial foot amputation in diabetic patients: a standardized method for evaluating bone margins with intraoperative culture. J Foot Ankle Surg. 2012;51:749–52. [PubMed] [Google Scholar]
8. Borkosky SL, Roukis TS. Incidence of re-amputation following partial first ray amputation associated with diabetes mellitus and peripheral sensory neuropathy: a systematic review. Diabet Foot Ankle. 2012;3:12169.[PMC free article] [PubMed] [Google Scholar]
9. Wong KL, Nather A, Lim J, Kuang SL. Clinical outcomes of diabetic foot patients following ray amputation. Poster; Sixth International Symposium on the Diabetic Foot in Noordwijkerhout; 11–14 May 2011; The Netherlands. 2011. [Google Scholar]
10. Brown ML, Tang W, Patel A, Baumhauer JF. Partial foot amputation in patients with diabetic foot ulcers. Foot Ankle Int. 2012;33:707–16. [PubMed] [Google Scholar]
11. Anthony T, Roberts J, Modrall JG, Huerta S, Asolati M, Neufeld J, et al. Transmetatarsal amputation: assessment of current selection criteria. Am J Surg. 2006;192:e8–11. [PubMed] [Google Scholar]
12. Pollard J, Hamilton GA, Rush SM, Ford LA. Mortality and morbidity after transmetatarsal amputation: retrospective review of 101 cases. J Foot Ankle Surg. 2006;45:91–7. [PubMed] [Google Scholar]
13. McCallum R, Tagoe M. Transmetatarsal amputation: a case series and review of the literature. J Aging Res. 2012;2012:797218.[PMC free article] [PubMed] [Google Scholar]
14. Elsharawy MA. Outcome of midfoot amputations in diabetic gangrene. Ann Vasc Surg. 2011;25:778–82. [PubMed] [Google Scholar]
15. Schade VL, Roukis TS, Yan JL. Factors associated with successful Chopart amputation in patients with diabetes: a systematic review. Foot Ankle Spec. 2010;3:278–84. [PubMed] [Google Scholar]
16. Pinzur MS. Restoration of walking ability with Syme's ankle disarticulation. Clin Orthop Relat Res. 1999;361:71–5. [PubMed] [Google Scholar]
17. Jany RS, Burkus JK. Long-term follow up of Syme amputations for peripheral vascular disease associated with diabetes mellitus. Foot Ankle. 1988;9:107–10. [PubMed] [Google Scholar]
18. Laughlin RT, Chambers RB. Syme amputation in patients with severe diabetes mellitus. Foot Ankle. 1993;14:65–70. [PubMed] [Google Scholar]
19. Pinzur MS, Stuck RM, Sage R, Hunt N, Rabinovich Z. Syme ankle disarticulation in patients with diabetes. J Bone Joint Surg Am. 2003;85-A:1667–72. [PubMed] [Google Scholar]
20. Harris RI. Syme's amputation; the technical details essential for success. J Bone Joint Surg Br. 1956;38:614–32. [PubMed] [Google Scholar]
21. Taniguchi A, Tanaka Y, Kadono K, Inada Y, Takakura Y. Pirogoff ankle disarticulation as an option for ankle disarticulation. Clin Orthop Relat Res. 2003;(414):322–8. [PubMed] [Google Scholar]
22. Altindas M, Kilic A. Is Boyd's operation a last solution that may prevent major amputations in diabetic foot patients? J Foot Ankle Surg. 2008;47:307–12. [PubMed] [Google Scholar]
23. Langeveld AR, Oostenbroek RJ, Wijffels MP, Hoedt MT. The Pirogoff amputation for necrosis of the forefoot: a case report. J Bone Joint Surg Am. 2010;92:968–72. [PubMed] [Google Scholar]
24. den Bakker FM, Holtslag HR, van den Brand JG. Pirogoff amputation for foot trauma: an unusual amputation level: a case report. J Bone Joint Surg Am. 2010;92:2462–5. [PubMed] [Google Scholar]
25. Nather A. The role of Pirogoff's amputation in treating diabetic foot infections. Poster; 42nd Malaysian Orthopaedic Association Annual General Meeting and Annual Scientific Meeting; 14-18 June 2012; Held in Kuantan, Malaysia. [Google Scholar]
Articles from Diabetic Foot & Ankle are provided here courtesy of Taylor & Francis
